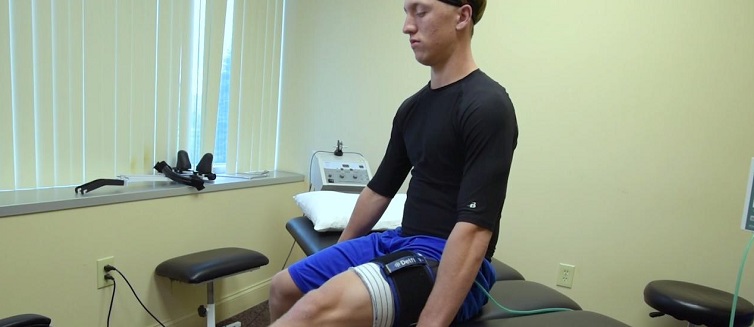
Blood flow restriction rehabilitation, or BFR, is an approach to rehabilitating muscle injuries, particularly those occurring in an arm or leg.
The specialized treatment method uses an FDA-approved surgical tourniquet system that looks very similar to a blood pressure cuff. The system is placed on an injured arm or leg. It periodically reduces blood flow to the limb while the patient performs specific exercises.
Limiting blood flow to the muscles (a process called occlusion) allows the patient to work the muscles without placing excessive weight on the limb. The use of BFR can vary throughout treatment.
“We are constantly studying state-of-the-art clinical practices and the latest research to benefit our patients,” says Jim Burns, PT, facility director at the UPMC outpatient rehabilitation location in Uniontown. “BFR is one of the newer tools that we’ve been able to add to our toolbox, and we have seen extreme benefits from this form of rehabilitation.”
Never Miss a Beat!
Learn more about the UPMC Centers for Rehab Services in our email newsletter
Thank you for subscribing!
You can now select the specific newsletters you'd like to receive.
You are already subscribed.
Subscribe to more newsletters in our email preference center.
Sorry, an error occurred. Please try again later.
Get Healthy Tips Sent to Your Phone!
Who Benefits from Blood Flow Restriction Rehabilitation?
Patients with most types of muscular injuries can receive BFR. That includes patients recovering from:
- Fractures that don’t grow back together or heal properly.
- Anterior cruciate ligament (ACL) injuries.
- Rotator cuff injuries.
- Achilles tendon injuries.
“Blood flow restriction therapy can benefit virtually every patient that we see,” Burns says. “Our patients with ACL reconstruction, nonunion fractures, tendon apathy, and tendon repair have all benefited from this form of rehabilitation.”
Older patients have also experienced significant benefits from BFR, Burns says.
“Some folks may have difficulty navigating stairs, getting into or out of a chair, or completing other basic activities during everyday life,” he says. “By providing this type of technology to our patients, we can help them improve and meet their goal.”
How Does Blood Flow Restriction Rehabilitation Work?
BFR forces the body to activate all muscles on the limb where the blood flow is restricted. It can be incorporated into traditional physical therapy sessions, just as other techniques or equipment might be.
“We’ll first have the patient work the injured muscle through traditional, weight-bearing physical therapy exercises, and then end with BFR,” Burns says. “This ensures the injured muscles have been worked to their fullest and, ultimately, can aid in faster recovery times.”
According to Burns, the science behind BFR is low-load training with heavy load benefits.
“So, strength gains are really based in heavy loads,” he says. “The safety of blood flow restriction allows very low loads to be applied to limbs and to the joints, yet patients are gaining the benefits of higher load lifting.”
For more information about blood flow restriction rehabilitation, call 1-888-723-4277 or visit our website.
Editor's Note: This video was originally published on , and was last reviewed on .
About UPMC Rehabilitation Institute
The UPMC Rehabilitation Institute offers inpatient, outpatient, and transitional rehabilitation, as well as outpatient physician services so that care is available to meet the needs of our patients at each phase of the recovery process. Renowned physiatrists from the University of Pittsburgh Department of Physical Medicine and Rehabilitation, as well as highly trained physical, occupational, and speech therapists, provide individualized care in 12 inpatient units within acute care hospitals and over 80 outpatient locations close to home and work.