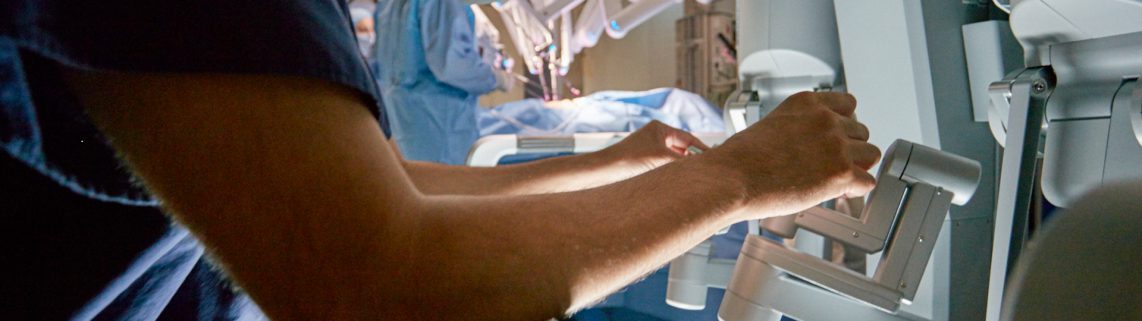
A recent UPMC research study suggests that combining robotic surgery and enhanced recovery protocols can result in shorter hospital stays for patients who undergo one of medicine’s most complex procedures: pancreatoduodenectomy.
Pancreatoduodenectomy (PD), also known as a Whipple procedure, is a highly complex surgical operation used to treat pancreatic cancer, pancreatitis, bile duct cancer, duodenal cancer, or other conditions causing pancreatic inflammation. It is a difficult procedure that can involve the removal of the head of the pancreas, the duodenum, the distal bile duct, or a combination of the three. The Whipple procedure, which can take hours to perform, is one of the most challenging abdominal surgeries, with a complication rate approaching 30 to 40 percent.
In leading edge medical centers, new approaches are always being explored to address the challenges of PD. Recent studies at UPMC indicate that two familiar and frequently used innovations — robotic surgery and Enhanced Recovery After Surgery (ERAS) — produce better patient outcomes when used together.
Never Miss a Beat!
Subscribe to Our HealthBeat Newsletter!
Thank you for subscribing!
You can now select the specific newsletters you'd like to receive.
You are already subscribed.
Subscribe to more newsletters in our email preference center.
Sorry, an error occurred. Please try again later.
Get Healthy Tips Sent to Your Phone!
Robotic Surgery: Extending the Surgeon’s Reach
Robotic techniques are minimally invasive procedures that can help reduce the trauma and invasiveness of traditional open-abdominal surgery for PD. “Robotic surgery is what people call it, but that’s really a misnomer,” says Amer H. Zureikat, MD, chief of the Division of Gastrointestinal Surgical Oncology at UPMC Hillman Cancer Center. “The ‘robot’ is actually a computer platform with tools that guide the surgeon’s hand. It gives you magnification, accuracy, and stability so you can do the surgery without opening the abdomen.”
Nearly 600 robotic Whipple procedures have been performed at UPMC since 2008, when it began studying the benefits of this less invasive approach for PD surgery. The results are encouraging: Dr. Zureikat’s team found that complication rates for the robotic Whipple were nearly 30 percent less when compared to nationwide statistics for the traditional open version of the procedure.
ERAS: Focusing on Recovery from the Beginning
But a reduction in complications alone doesn’t lead to shorter hospital stays. Dr. Zureikat is studying ERAS as another innovation to help patients get back on their feet sooner.
Over the last decade, ERAS has been associated with reductions in length of hospital stay and cost across a wide range of surgical specialties, including colorectal, urologic, and bariatric procedures. Increasingly, ERAS pathways are being applied to pancreatic surgery on the theory that it can be even more beneficial for these complex procedures.
ERAS care plans are structured, evidence-based pathways designed to limit physiological stress and expedite patient recovery. They commonly focus on three aspects of care after surgery: the use of more than one method for pain management, the early delivery of food (usually through a feeding tube), and a focus on getting patients out of bed and engaged in light activity as soon as possible.
At UPMC, ERAS care minimizes the use of narcotics for pain management, favoring alternatives wherever possible. With lower levels of narcotics in their system, patients are able to digest food and get exercise sooner after surgery, speeding recovery. UPMC’s pioneering application of the ERAS protocol for PD limits narcotics to a single spinal dose of morphine for surgery, followed by alternative pain relief.
Dr. Zureikat’s study demonstrated that UPMC’s ERAS implementation protocol is safe, feasible, and beneficial for both open and robotic pancreatoduodenectomy. ERAS decreased post-operative length of stay without impacting complications or readmissions, and was associated with a cost savings of nearly $4,000 per patient.
One Plus One Is Three
What is most interesting to Dr. Zureikat and his research team is the apparent synergy these two innovations create when applied together in PD cases. The study, which compared length of stay statistics for various combinations of robotic surgery and ERAS, indicated that applying the two together may provide the optimal condition for improved PD outcomes.
Dr. Zureikat cautions that more research is necessary to verify these results, which are based on a small sampling of cases. Nevertheless, the indicators are there. “It could be a case of one plus one equals three,” says Dr. Zureikat. He theorizes that the additional benefit may be due to the additive effect that minimally invasive surgery has on limiting physiologic stress and preserving immune function, in addition to the known benefits of ERAS management.
It all adds up to a quicker recovery and a shorter hospital stay for PD patients. “It’s not just the cost,” adds Dr. Zureikat. “A shorter stay in the hospital gets patients back to work, back to their families, and back to their lives sooner. It’s just better medicine.”
Editor's Note: This article was originally published on , and was last reviewed on .
About UPMC
Headquartered in Pittsburgh, UPMC is a world-renowned health care provider and insurer. We operate 40 hospitals and 800 doctors’ offices and outpatient centers, with locations throughout Pennsylvania, Maryland, New York, West Virginia, and internationally. We employ 4,900 physicians, and we are leaders in clinical care, groundbreaking research, and treatment breakthroughs. U.S. News & World Report consistently ranks UPMC Presbyterian Shadyside as one of the nation’s best hospitals in many specialties and ranks UPMC Children’s Hospital of Pittsburgh on its Honor Roll of America’s Best Children’s Hospitals. We are dedicated to providing Life Changing Medicine to our communities.