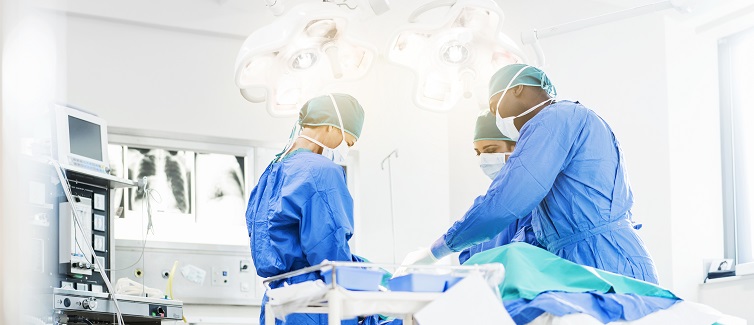
Experts at UPMC Passavant use state-of-the-art technology to offer the most advanced surgical treatment options to North Hills area residents
With two convenient campuses in McCandless and Cranberry Township, UPMC Passavant offers a wide range of services and care much closer to home.
Never Miss a Beat!
Subscribe to Our HealthBeat Newsletter!
Thank you for subscribing!
You can now select the specific newsletters you'd like to receive.
You are already subscribed.
Subscribe to more newsletters in our email preference center.
Sorry, an error occurred. Please try again later.
Get Healthy Tips Sent to Your Phone!
The Benefits of Robotic-Assisted Surgery
Thanks to advanced, robotic-assisted technology, surgeons at UPMC Passavant provide patients with more minimally invasive treatment options in cancer, general surgery, neurology, women’s health, and more.
Robotics allow doctors to make smaller cuts, more precise movements, and maintain complete control over each action. While this technology is beneficial to surgeons, it mostly benefits patients because of its minimally invasive technique. Robotic-assisted surgery benefits patients as well because the minimally invasive technique can lead to fewer complications, faster recoveries, and less time spent in the hospital.
“Whenever possible, we select the least invasive procedure that would result in the greatest outcome for the patient — focusing on greatly improving their symptoms,” says Robert Bailey, MD, a neurosurgeon in the UPMC Department of Neurosurgery, who see patients in Butler, New Castle, Sewickley, and Wexford.
Putting Technology into Practice
Kevin Garrett, MD, a surgeon and chair of the UPMC Department of General Surgery at UPMC Passavant–McCandless, focuses on robotic general surgeries for treating hernias, the gallbladder, and soft tissue, as well as emergency general procedures. Dr. Garrett and his team use robots in multiple minimally invasive surgeries to repair complex abdominal wall and groin hernias and remove gallbladders.
The UPMC Passavant neurosurgery team offers patients a wide spectrum of treatments, including minimally invasive procedures like kyphoplasty, which treats compression fractures and abnormal configurations usually caused by osteoporosis. The surgery has high success rates for:
- Stopping pain caused by fractures
- Stabilizing the bone
- Restoring some or all vertebral body height lost due to compression
“Our minimally invasive surgical procedures include a microdiscectomy where patients are able to go home the same day,” says Matt El-Kadi, MD, PhD, chief of neurosurgery at UPMC Passavant and director of the UPMC Spine Center. A microdiscectomy treats patients with “pinched” nerves in the spinal column caused by herniated or ruptured discs.
Fighting Cancer with Innovative Surgical Treatments
Patients at UPMC Passavant have access to the experts and care found at the renowned UPMC Hillman Cancer Center, which offers one of the world’s largest and most comprehensive programs in robotic cancer surgery.
In 2020, UPMC Passavant introduced a minimally invasive alternative to traditional open surgery for liver resection procedures, which entails cutting out the liver to cure liver cancer.
“This technology means more patients can receive the benefits of minimally invasive surgery. In general, they have less pain, enjoy a shorter hospital stay, and experience faster recovery,” says David Geller, MD, director of the UPMC Liver Cancer Center.
Several features of the robotic technology contribute to a more precise and efficient surgery, including:
- A magnified 3D view of the patient’s anatomy.
- The ability to use tiny arms and instruments in the procedure.
- The robotic arms never become fatigued.
Even though the surgeons utilize a minimally invasive technique, liver surgery is a complex procedure that requires a group of experienced surgical oncologists, nurses, technicians, and anesthesiologists working together in the operating room (OR).
“It takes a lot of orchestration in the OR to perform. We work as a team to take care of the patient,” says Melanie Ongchin, MD, chief of surgical oncology at UPMC Passavant.
According to Samer Tohme, MD, a surgical oncologist who leads the program at UPMC Passavant–McCandless, the team has completed 30 procedures since August 2020.
Dr. Geller adds, “We’re providing a full-scale service for liver evaluation, surgery, and follow-up care. And it’s right in our patients’ backyards.”
In the same year, UPMC Passavant–McCandless became the first hospital in the Pittsburgh area to use the Monarch™ robotic bronchoscopy system. It allows doctors to more easily maneuver into the lung’s tiniest passages to inspect suspicious lesions and collect tissue samples to determine whether they are cancerous or benign. The technology combines the latest advancements in robotics, software, and data science with minimally invasive endoscopy, which uses small cameras and tools to enter the body through the patient’s mouth — allowing for earlier, more precise detection of cancer.
“Early diagnosis is critical,” says Ryan Levy, MD, chief of thoracic surgery at UPMC Passavant and thoracic surgeon with UPMC Hillman Cancer Center. “When lung cancer is detected at an earlier stage, we’re able to offer our patients more treatment options — meaning patients have better outcomes and increased cancer-free rates.”
In addition to liver and lung cancer operations, UPMC Passavant surgical oncologists use robotic techniques in various procedures, such as:
- Pancreaticoduodenectomy, also known as a Whipple procedure, to treat pancreatic cancer.
- Hyperthermic intraperitoneal chemoperfusion (HIPEC) to treat peritoneal carcinomatosis, a rare type of cancer that can develop when gastrointestinal or gynecologic cancers spread.
Highly Specialized Surgical Services for Women
At UPMC Passavant, UPMC Magee-Womens Specialty Services offer comprehensive women’s health care, including state-of-the-art surgery.
Robert Edwards, MD, is chair of the UPMC Department of Obstetrics, Gynecology, and Reproductive Sciences at UPMC Magee-Womens Hospital, co-leader of the UPMC Gynecologic Cancer Program, and a surgeon at UPMC Passavant. He sees patients at both UPMC Passavant locations and in Oakland at UPMC Magee-Womens Hospital.
His research focuses on ovarian cancer and how to better design treatments that combine surgery, chemotherapy, and immunotherapy to prevent cancer from coming back. “Whether it’s making a first attempt at removing the disease using surgery or performing surgery after reducing some of the cancer with chemotherapy, we can usually get about 80 percent of patients cancer free,” says Dr. Edwards.
When it comes to gynecologic cancer surgery, more than 50% of the cases are done laparoscopically.
“Ovarian cancer is unique amongst solid tumors in that it can be removed by surgery, particularly at the first signs of it, and may require several hours to extract the tumor,” says Dr. Edwards.
Patients who undergo minimally invasive procedures like this typically experience the following advantages:
- Less bleeding and scarring
- Reduced pain
- Shorter hospital stays
- Quicker recovery
- Earlier returns to normal activity
- Smaller scars
In addition to delivering high-end surgical treatments for patients with gynecologic malignancies, UPMC Passavant’s four gynecologic oncologists provide comprehensive care. They offer the latest in cancer prevention, detection, diagnosis, other treatments, such as chemotherapy, and staging, as well as access to experimental treatment options and clinical trials.
Dr. Edwards adds, “With the team-based cancer care, UPMC Passavant is very impressive.”
* Monarch™ is a trademark of Auris Health, Inc.
Editor's Note: This article was originally published on , and was last reviewed on .
About UPMC
Headquartered in Pittsburgh, UPMC is a world-renowned health care provider and insurer. We operate 40 hospitals and 800 doctors’ offices and outpatient centers, with locations throughout Pennsylvania, Maryland, New York, West Virginia, and internationally. We employ 4,900 physicians, and we are leaders in clinical care, groundbreaking research, and treatment breakthroughs. U.S. News & World Report consistently ranks UPMC Presbyterian Shadyside as one of the nation’s best hospitals in many specialties and ranks UPMC Children’s Hospital of Pittsburgh on its Honor Roll of America’s Best Children’s Hospitals. We are dedicated to providing Life Changing Medicine to our communities.