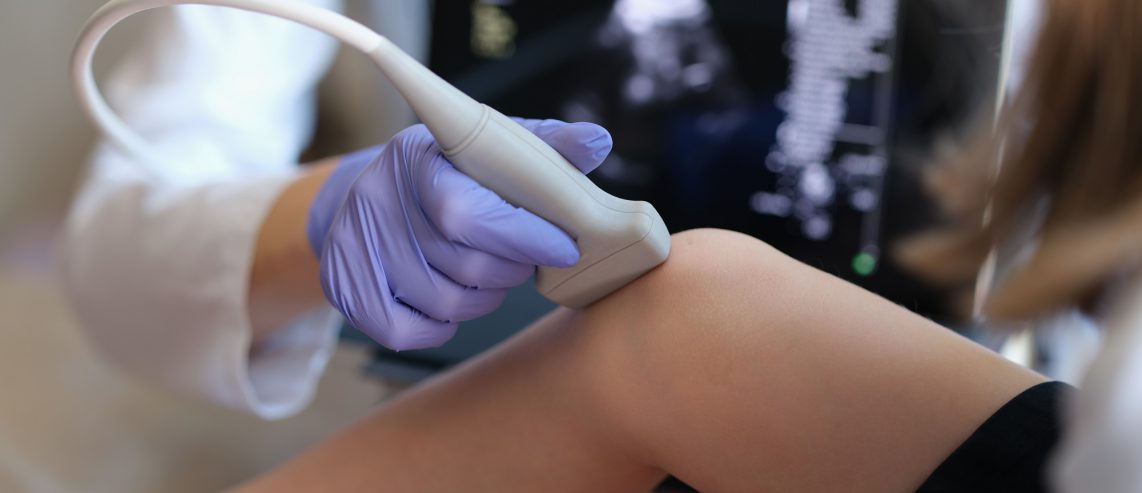
Point-of-care ultrasound is a focused ultrasound exam. A clinician performs this exam at a person’s bedside. They do this to speed up decision-making and answer specific questions in real time.
The UPMC Children’s Hospital of Pittsburgh point-of-care ultrasound, or POCUS, program started in 2015. The program’s aim is to improve the accuracy, quality, and efficiency of clinical care.
It’s one of only a few of its kind nationwide.
The program involves more than a dozen medical specialties. These include anesthesia, critical care, emergency medicine, pediatric surgery, ophthalmology, and urology.
Point-of-care ultrasound is a powerful tool that allows for dynamic round-the-clock assessment. It allows for this even in areas without quick, easy access to x-rays or CT scans.
Here’s what to know about point-of-care ultrasound and its benefits.
Never Miss a Beat!
Subscribe to Our HealthBeat Newsletter!
Thank you for subscribing!
You can now select the specific newsletters you'd like to receive.
You are already subscribed.
Subscribe to more newsletters in our email preference center.
Sorry, an error occurred. Please try again later.
Get Healthy Tips Sent to Your Phone!
Benefits of Point-of-Care Ultrasound
Clinicians increasingly use point-of-care ultrasonography. They do this to give accurate, timely diagnoses and help guide procedures. That’s according to the American Academy of Pediatrics.
Clinicians have performed ultrasonography since the 1960s. This was when obstetricians and cardiologists first used it.
Clinicians can perform (and repeat) these exams at all hours. There’s no need to transport a person to another department for screening.
There’s also no ionizing radiation exposure. The technology relies on sound waves — not x-rays — to generate images.
It may direct further evaluation and avoid unnecessary or costly testing, too.
How Do Clinicians Use Point-of-Care Ultrasound?
Point-of-care ultrasound has many uses in pediatrics. This includes uses in emergency departments and for trauma cases. Repeat exams can allow for dynamic assessment and faster intervention.
Offering point-of-care ultrasound also improves the satisfaction of those receiving care.
“Emergency medicine has been using this for decades — since the 1980s — pretty consistently,” says Jennifer Marin, MD, MSc.
Dr. Marin is medical director of the POCUS program. She’s also director of Emergency Department Imaging at UPMC Children’s Hospital of Pittsburgh. “There are studies that have shown that accuracy of diagnoses is improved, that patient satisfaction is improved, and that length of stay is improved when this is used,” she adds.
“I will tell you, in addition to the evidence, anecdotally, our patients really appreciate it when we can do the exam at bedside and show them the images, explain it to them, and make a diagnosis quicker and potentially more accurately,” she says.
Point-of-care ultrasound isn’t only for emergency medicine, says Dr. Marin. It also helps standardize care and improve clinical accuracy in many specialties.
Dr. Marin took an interest in further developing the POCUS program. She did this while studying the Focused Assessment with Sonography in Trauma (FAST) exam.
“This is an exam we do with bedside ultrasound for trauma patients, looking for free fluid,” she says.
Certain bedside ultrasounds are unnecessary, Dr. Marin says. This is because UPMC Children’s Hospital offers 24-hour radiology ultrasound and a top-tier ultrasound staff.
“But in our emergency department — and I can speak to other divisions that are using the technology — we find that it is really useful for evaluating soft tissue infections, whether there’s an abscess or cellulitis,” she says. “We do it pretty routinely for patients that are limping or have hip pain to know if there’s an effusion as the cause of their pain.
“We also do it for procedural guidance, ultrasound-guided peripheral IVs. We use it for cardiac function, pericardial effusion (extra fluid buildup around the heart) for trauma patients — for patients who are hypotensive or who have unexplained tachycardia and we want to know the reasons for why they’re in shock,” she says.
The UPMC Children’s Hospital POCUS program includes more than a dozen pediatric subspecialties. They include:
- Anesthesia
- Cardiac anesthesiology
- Cardiac critical care
- Critical care medicine
- Emergency medicine
- Nephrology
- Newborn medicine
- Ophthalmology
- Pediatric and adolescent gynecology
- Pediatric neurology
- Pediatric surgery
- Rheumatology
- Urology
- Vascular access team
The program’s mission is to improve patient care across clinical specialties. It does this by standardizing point-of-care diagnostic and procedural ultrasound performance. “I think, if we were to sum it up, it would be for a patient where you really need the information pretty quickly,” says Dr. Marin. “You can incorporate it into your clinical examination. And it’s also a really nice tool because we can repeat it.”
To learn more information about the POCUS program, visit CHP.edu/Our-Services/POCUS.
For more about UPMC Children’s Hospital of Pittsburgh, visit www.chp.edu.
About Pediatrics
From nutrition to illnesses, from athletics to school, children will face many challenges growing up. Parents often will make important health care decisions for them. We hope to help guide both of you in that journey. UPMC Children’s Hospital of Pittsburgh is a national leader in pediatric care, ranking consistently on U.S. News & World Report’s Best Children’s Hospitals Honor Roll. We provide expert treatment for pediatric diseases, along well-child visits, urgent care, and more. With locations across Pennsylvania, Maryland, and West Virginia, you can find world-class care close to home. We also work closely with UPMC Magee-Womens Hospital, a national leader in care for newborns and their mothers. Our goal is to provide the best care for your children, from birth to adulthood and beyond. Visit our website to find a doctor near you.